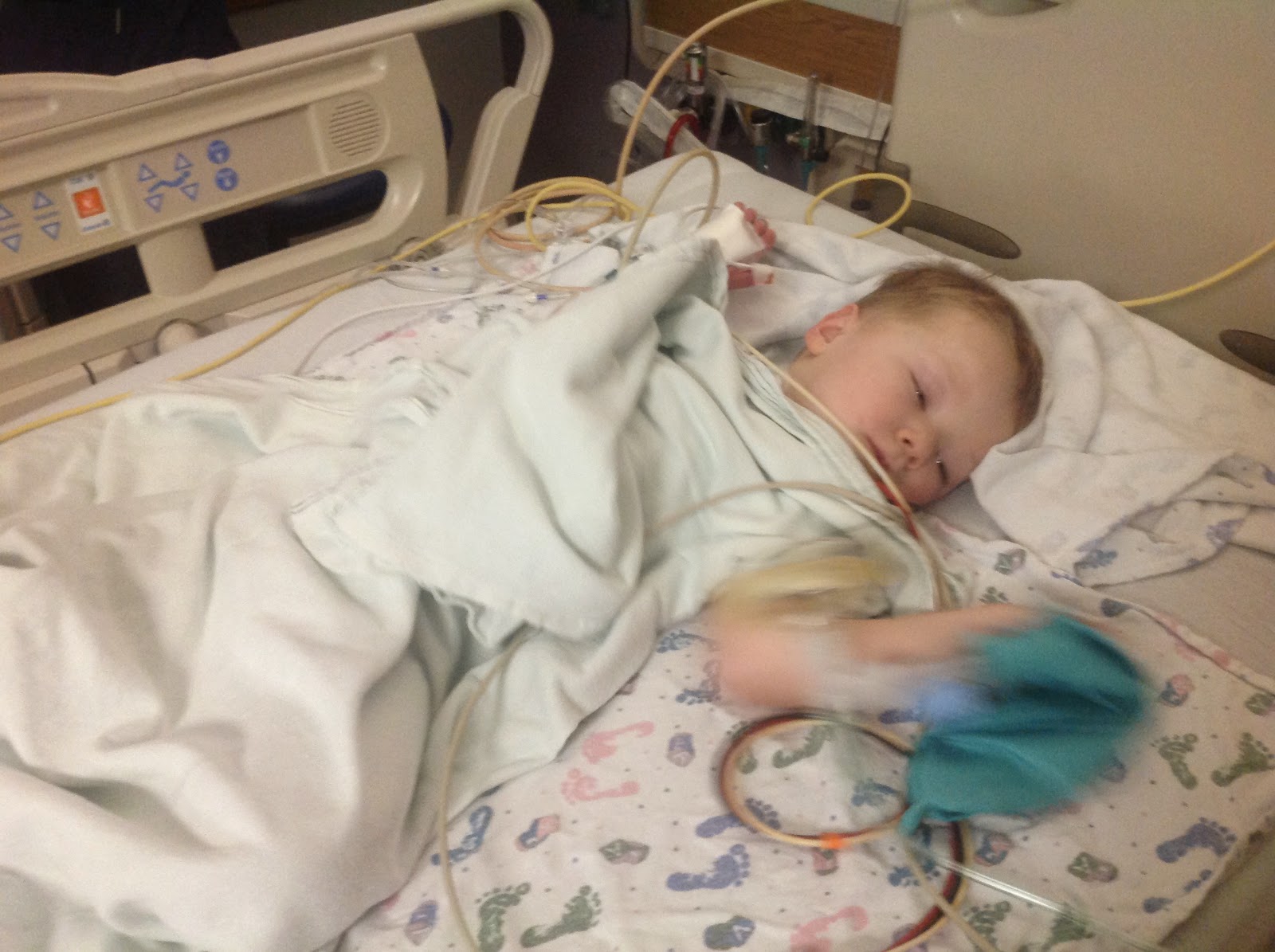
We have been home for five days and things are starting to go back to normal!
We visited the cardiologist in a Boise yesterday and things looks pretty good. They did a transthorasic echocardiogram, EKG, and physical check up. In the echo the fenestration (small hole between the new vena cava conduit and the atrium) had a pressure gadiant of 7-8. This is not unexpected because of the elevated pressures in the heart prior to Fontan surgery. However it is higher than ideal (hoping for a 5). There was no fluids leaking around the heart, which is a good sign. His oxygen saturations were about 92% so the cardiologist opted to stop oxygen. He decreased the lasix to once a day and said to only give pain medications when Luke is in pain. It has been about 30 hours since the last pain medication dose and Luke is fine, even laughing.
We still cannot submerge his incision or chest tube sites. He is sometimes acting lethargic, asking for bed at nap time and night. But I hear it is a good 4 weeks before post Fontan kids start to show improvements from prior to surgery.
It is wonderful to be a family together again. Thank you for all of the wonderful meals, mom getting my kids off to school, support,, and everything.
Luke is our fifth child and he was born with Hypoplastic Left Heart Syndrome. His life has been a roller coaster thus far. We want to share our experience with him for friends, family, and other HLHS families.
Before Surgery- no chest scars

Saturday, February 21, 2015
Tuesday, February 17, 2015
We Are Home!
We got home about 9:30 last night. We had to wait for six hours at the hospital, after discharge, for oxygen to be set up. When we got home there was no oxygen on the doorstep so I had to make a few phone calls and bring the poor Norco RT out For a delivery late at night. But we made it and we are glad to be here.
Luke is super clingy and wants to be on my lap all the time. I though I would be getting lots done but I won't. It's all about him right now anyway.
Thank you everyone for your prayers, fasting, love and support. They are a great power and I know they have helped Luke through the first parts of this ordeal.
Luke is super clingy and wants to be on my lap all the time. I though I would be getting lots done but I won't. It's all about him right now anyway.
Thank you everyone for your prayers, fasting, love and support. They are a great power and I know they have helped Luke through the first parts of this ordeal.
Sunday, February 15, 2015
4 Days Post Op
Luke had his last IV line pulled today. His chest X-ray showed less fluids. He walked around a lot. He had a bowel movement after 5 days of nothing. That has helped his stomach to hurt less. He hasn't had anything for pain since early in the morning. He hates the taste of the medicine so I think he is just baring the pain to avoid the medicine. But he hardly complains. My poor, tough boy.
He is still on 3/4 liter of oxygen. We will probably go home with oxygen. He had an Echocardiogram which showed continued elevated pressures in the atrium and pulmonary arteries. They are hopeful that the lower elevations of Boise will help with that. If not the cardiologist in Boise will prescribe Syldinafil (Viagra) again. That was a pain to give because it was three times a day and tastes awful.
We have been told we will go home tomorrow as long as the X-ray is clean. I hope it's true.
Saturday, February 14, 2015
3 Days Post Operative
Both of the chest tubes came out today! Luke has been up walking and eating some. His chest x-Rays are still cloudy so we need to get him moving, coughing, and keep up with the lasix. The bandage is off his incision site and I have included a picture of that. Mark went home today for Isaac's birthday celebration. Luke was very sad to see him go. He wanted me to go and daddy to stay with him.
Friday, February 13, 2015
Onto the Floor and Out of the ICU 2/13/15
Luke was moved onto the floor today and out of the ICU, which is a major step to being discharged. They pulled the mediastinal chest tube. All medications except his lasix are now oral. His chest x-Ray from this morning was still cloudy so they are working on getting higher liquid outputs. Luke is eating pretty well. His itches have finally gone away. Yesterday he could barely sit still because he was itching his whole body as a side effect of the morphine. He hasn't needed Benadryl for 12 hours. He walked for the first time and did a great job of it.
We had a small scare this morning. The surgeon sent a specialist in to evaluate if Luke needed to go back into surgery and have a pacer installed. With his recent incision his chest would open easily and the scar tissue wouldn't be a factor. The specialist determined Luke does have SA Node dysfunction. But she believes that it will be a few years before he will need a pacer. This really frightens me because I was hoping that the Fontan would fix Luke until he needed a transplant in his 20s. Instead, he will probably have his chest opened again before he is 10. Oh how I wish I could undergo the operations for him!
Here are some pictures from the day.
We had a small scare this morning. The surgeon sent a specialist in to evaluate if Luke needed to go back into surgery and have a pacer installed. With his recent incision his chest would open easily and the scar tissue wouldn't be a factor. The specialist determined Luke does have SA Node dysfunction. But she believes that it will be a few years before he will need a pacer. This really frightens me because I was hoping that the Fontan would fix Luke until he needed a transplant in his 20s. Instead, he will probably have his chest opened again before he is 10. Oh how I wish I could undergo the operations for him!
Here are some pictures from the day.
38 Hours Post Operative 2/13/15
Yes it is Friday the 13th. But we are hopeful nothing untoward will happen.
Luke has slept through the night. The nurse has not given him any pain medications since 11:00 p.m. I am worried that when he awakens he will be in a lot of pain.
Yesterday they removed his IJ (intra jugular) and the arterial line in his right wrist. He was able to stand up for a moment and to sit in dad's lap for a few hours. Today the nurse practitioner says his largest chest tube (the mediastinal) can come out. They want to leave in the two small chest tubes (ponytails) until Luke has eaten more fats. In surgery there is a possibility of splicing a lymph node. This is undetectable until the patient eats fats, then fats drain into the chest cavity, and they drain out from the chest tubes. If this is the case Luke would be on a no fat diet for a few weeks. So far the chest drainage appears clear but he has not eaten enough to know for sure. We will try and urge him to eat nice fatty foods today. Lucky guy!
Luke has slept through the night. The nurse has not given him any pain medications since 11:00 p.m. I am worried that when he awakens he will be in a lot of pain.
Yesterday they removed his IJ (intra jugular) and the arterial line in his right wrist. He was able to stand up for a moment and to sit in dad's lap for a few hours. Today the nurse practitioner says his largest chest tube (the mediastinal) can come out. They want to leave in the two small chest tubes (ponytails) until Luke has eaten more fats. In surgery there is a possibility of splicing a lymph node. This is undetectable until the patient eats fats, then fats drain into the chest cavity, and they drain out from the chest tubes. If this is the case Luke would be on a no fat diet for a few weeks. So far the chest drainage appears clear but he has not eaten enough to know for sure. We will try and urge him to eat nice fatty foods today. Lucky guy!
Thursday, February 12, 2015
RA and Foley removed 11:30 a.m.
The nurse practitioner just removed his RA or right atrial line and the nurse his Foley catheter. They had to give Ativan because he was so worried about being worked on. He is resting now but not sleeping. He didn't sleep much, only about 3 hours last night so he is very tired.
This picture shows the RA, white line, just before removal. It was about 6-8 inches long inside of him.
This picture shows the RA, white line, just before removal. It was about 6-8 inches long inside of him.
19 Hours Post Op 2/12/15
Last night they kept Luke well sedated with Versed for anxiety/relaxation and morphine and Tylenol for pain. Today they have changed the morphine to oxicodone which is an oral narcotic for pain. They just stopped the Milrinone which is a heart med that helps with the hearts contraction and dilates the vessels to help the blood flow easier. This med won't be out of Luke's system for about 6 hours so they are going to reevaluate him at that point.
He is still on the pacer, set to go off when his heart rate falls below 82 beats per minute. He has not fallen that low for a long time. His chest x-Ray showed a bit of cloudiness in the left lung lobes. They are increasing his lasix to help him urinate that off. They feel the cloudiness is just from excess fluids still on board and not indicative of pneumonia.
Luke is awake, drinking, and full of demands. He has requested lots of toys that he has played with in the hospital from the last few days. I got to go on a scavenger hunt and try to round them up. He is watching tv and seems content.
He is still on the pacer, set to go off when his heart rate falls below 82 beats per minute. He has not fallen that low for a long time. His chest x-Ray showed a bit of cloudiness in the left lung lobes. They are increasing his lasix to help him urinate that off. They feel the cloudiness is just from excess fluids still on board and not indicative of pneumonia.
Luke is awake, drinking, and full of demands. He has requested lots of toys that he has played with in the hospital from the last few days. I got to go on a scavenger hunt and try to round them up. He is watching tv and seems content.
Wednesday, February 11, 2015
Post operative first visit
Here are some pictures of Luke as he looks post op. One is a close up of his face. Notice the pink lips. They have been blue for so long that the change is amazing!
The surgery is done! They just finished stitching Luke back up. We will see him in a few more minutes. All told surgery lasted about 6 1/2 hours. Most of the time (3 hours) was just cutting through all of the scar tissue.
The surgeon said that Luke has hundreds of collaterals all over his heart. But hopefully with this new blood flow they will decrease in size. Luke had to be paced for a while as they were taking him off the bypass machine because of a slow heart rate. This could be because of the anesthetics or it could be indicative of problems with the SA Node. If that is the case he will get a pace maker some day. I sure hope not (10-15% of kids with the Fontan get a pacer).
The surgeon said that Luke has hundreds of collaterals all over his heart. But hopefully with this new blood flow they will decrease in size. Luke had to be paced for a while as they were taking him off the bypass machine because of a slow heart rate. This could be because of the anesthetics or it could be indicative of problems with the SA Node. If that is the case he will get a pace maker some day. I sure hope not (10-15% of kids with the Fontan get a pacer).
Here is the gortex conduit that they attached to the inferior vena cava and the right pulmonary artery. It is a 20 gauge size, flexible, and stretchable. See the small hole at the top. That is the size of the fenestration or small hole going through the synthetic inferior vena cava to the atrium, acting as a release valve for high pressures.
Fontan Surgery 2/11/15
We checked into Primary Children's hospital at 7:00. Luke was again fasting. He had to have a bath the night before, have a special antiseptic wipe rub-down, and a nasal swab. This was repeated this morning. All new measures to help cut down on infections post operatively.
Before surgery we had another physical, visited with Dr. Burch the surgeon, Dr Greenwood the anesthesiologist, the attending P.A., and other staff. Luke kept saying "I hate this" and "I want to go home now!" I guess yesterday's cardiac cath left some bad memories.
They gave him some Versed 20 minutes before taking him to he O.R. room. Mark and I hugged and kissed him goodbye. Here is a picture of our sleepy-eyed boy as he was leaving us.
Before surgery we had another physical, visited with Dr. Burch the surgeon, Dr Greenwood the anesthesiologist, the attending P.A., and other staff. Luke kept saying "I hate this" and "I want to go home now!" I guess yesterday's cardiac cath left some bad memories.
They gave him some Versed 20 minutes before taking him to he O.R. room. Mark and I hugged and kissed him goodbye. Here is a picture of our sleepy-eyed boy as he was leaving us.
Mark and I are in the waiting room. We have been told to expect 6 hours. We should get hourly updates. Thank you to everyone for your love and support!
Tuesday, February 10, 2015
Cardiac cath 2/10/15
Luke had a cardiac cath today. He had to be fasting food for 8 hours and no fluids 3 hours pre op. We got to the hospital at 5:45 a.m. And the procedure started around 8:00.
Doctor Gray was the attending cath surgeon. He said the atrial, ventricular, and pulmonary artery pressures were all high. He found multiple collaterals and closed about three off on the right side of the heart. He said he left the one on the left side of the heart there because of tomorrow's Fontan surgery.
Collaterals are small blood vessels that form as the body tries to compensate for low oxygen saturations. Luke's were running from his aorta to the pulmonary arteries. The attending physician said about 50% of post Glenn kids develop collaterals. So it was not unexpected.
Here is Luke after being checked in but before surgery.
Here is Luke in the postoperative recovery room.
Doctor Gray was the attending cath surgeon. He said the atrial, ventricular, and pulmonary artery pressures were all high. He found multiple collaterals and closed about three off on the right side of the heart. He said he left the one on the left side of the heart there because of tomorrow's Fontan surgery.
Collaterals are small blood vessels that form as the body tries to compensate for low oxygen saturations. Luke's were running from his aorta to the pulmonary arteries. The attending physician said about 50% of post Glenn kids develop collaterals. So it was not unexpected.
Here is Luke after being checked in but before surgery.
Subscribe to:
Comments (Atom)